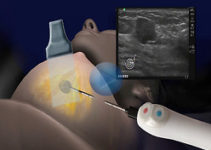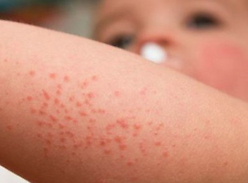
London, United Kingdom — Rates of hayfever and eczema are higher in children exposed to antibiotics in the first 2 years of life than in unexposed children, according to results from a systematic review and meta-analysis.
“We strongly suggest physicians take this into account when they prescribe antibiotics, especially for children in early life,” said lead investigator Fariba Ahmadizar, PharmD, from Utrecht University in the Netherlands.
For their meta-analysis, presented here at the European Respiratory Society International Congress 2016, Dr Ahmadizar and her colleagues examined cohort, case–control, and cross-sectional studies published between January 1966 and November 2015.
They looked at 21 studies involving 394,517 children with hayfever, 22 studies involving 229,080 children with eczema, and 12 studies involving 64,638 children with both.
Overall, early antibiotic exposure was associated with an increased risk for hayfever (odds ratio [OR], 1.23) and for eczema (OR, 1.26). The highest risks for hayfever and for eczema were seen in cross-sectional studies.
Table. Odds Ratio for Condition by Type of Study
| Type of Study | Hayfever | Eczema |
| Cohort | 1.18 | 1.24 |
| Case–control | 1.14 | 1.15 |
| Cross-sectional | 1.56 | 1.41 |
However, “we did not find any statistically significant difference between different study designs or the child’s age at exposure to antibiotics and diagnosis of allergies,” Dr Ahmadizar reported.
For both hayfever and eczema, the association was stronger in children treated with two or more courses of antibiotics than in those treated with just one course. The researchers did not have sufficient data to look at the association between each condition and type of antibiotic.
These findings might be explained by the immunomodulatory effect of antibiotics, said Dr Ahmadizar.
“Gut microbiota are thought to play an important role in the development of the immune system early in life, and reduced gut microbial diversity by exposure to antibiotics in early infancy leads to the imbalanced Th1 and Th2 response, which is related to an increased risk of allergies and other immune-related disorders,” she explained.
However, exposure to infection rather than treatment might also explain the results, she acknowledged.
“We also found an increased risk for food allergy by exposure to antibiotics in early life, but since we could only include three studies for this part of the meta-analysis, we did not include the results,” she added.
“These findings are important and may potentially explain the increase in allergic diseases, which coincides with an increase in antibiotic usage,” said Bryan Love, PharmD, from the South Carolina College of Pharmacy in Columbia.
Dr Love was involved in a recent study that revealed an association between early antibiotic exposure and food allergy (Allergy Asthma Clin Immunol. 2016;12:41).
“It is well known that antibiotics can disrupt the normal flora of the skin, respiratory system, and gastrointestinal tract, and researchers are just beginning to understand the potential effects that antibiotics may cause through alteration of the microbiome,” he explained.
“We know that microbes that colonize these areas contribute to immune development, and studies like this suggest that antibiotics may interfere with proper immune development, possibly leading to allergic diseases,” he added.
Dr Ahmadizar and Dr Love have disclosed no relevant financial relationships.
European Respiratory Society (ERS) International Congress 2016: Abstract P3639. Presented September 6, 2016.
Source: Kate Johnson, medscape.com